- Home >
- Prescription and Medication Error Claims
When you are unwell, you expect healthcare professionals to prescribe the right medicine to help you feel better. While the vast majority of prescriptions are issued and dispensed correctly, mistakes can happen.
If your GP prescribed the incorrect dosage, or your pharmacy gave the wrong medication, you may have a right to compensation. With over 30 years of specialist experience and millions recovered for clients affected by prescription negligence, our solicitors can pursue your case so you achieve a fitting settlement.
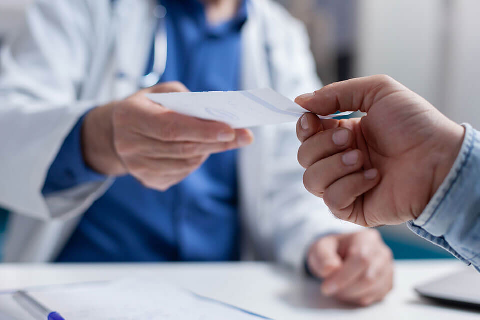
Do you have a medication error compensation claim?
Prescription and medication errors are thankfully rare. But when healthcare providers prescribe the wrong drug, mislabel medication or issue incorrect instructions, the consequences can be severe – from prolonging illnesses to causing severe allergic reactions.
If you or a loved one has been affected by a prescription error, our trusted team of solicitors are here to guide your claim. We tirelessly review all evidence and collaborate with impartial experts to build the strongest possible case and secure a settlement that protects your financial future.

The specialist prescription error claims solicitors for Essex & East Anglia
Since 1993, we have helped countless claimants secure the compensation and answers they were owed following avoidable errors involving their prescriptions or medication.
Through considered advice and a meticulous approach to investigation, our medical negligence solicitors make pursuing a case as seamless and stress-free as possible. We work on a ‘no win, no fee’ basis to remove any financial barriers to justice, with 96% of our cases settled outside the courtroom.
What does our medication error claim process look like?

A free initial consultation
Call us, request a callback or complete our online form and we’ll assess if you have a valid medical negligence claim.

Funding your claim
Discover the ways we can fund your claim without you paying a penny at any stage of the process.

Investigating evidence
We gather medical records, witness statements and more to learn what happened to you and prove your claim.

Instructing independent medical experts
We work with impartial, experienced medical experts to establish whether your injuries were due to substandard medical care.

Valuing your claim
We assess your health and financial losses to accurately estimate how much compensation your claim is worth.

Presenting your case
We contact the Defendants and the Courts on your behalf to set out your allegations and receive a response.

Negotiating a settlement
We work to achieve a fair settlement for you outside the courtroom – this is how 96% of our cases end.

Preparing for Trial
If we must proceed to Trial, we fully prepare you for what to expect so you receive the right result in court.
FAQs about prescription error negligence claims
What is a prescription error claim?
Over a billion prescription items are distributed each year across England. Most of this medicine is correctly prescribed by doctors and dispensed by pharmacists. However, like any other medical process, mistakes do occur.
While these instances are few and far between, patient safety data suggests medication errors are among the most common types of medical negligence. They typically fall into two main categories:
- Prescription errors, which happen when a GP or doctor issues the wrong dose, type or form of medication to an individual
- Dispensing errors, which arise when a pharmacist is to blame for a person receiving incorrect, ineffective or actively harmful medication
When a doctor, pharmacist or other medical professional makes one of these errors, affected individuals have the right to bring a claim and seek compensation. This can help them pay for replacement medication, fund further treatments and recoup any financial losses caused by this error, among other expenses.
If you were given the wrong prescription by a medical professional, or a pharmacist made a mistake when dispensing medication, our solicitors meticulously investigate every piece of evidence and consult impartial medical professionals to understand what happened to you.
What are the most common types of prescription errors?
According to recent research, approximately 237 million medication errors occur in England and Wales every year. Common prescribing errors include:
- Prescribing the incorrect dosage or frequency of medication
- Issuing the wrong format of drugs (e.g. prescribing a pill when a patient should take liquids)
- Prescribing drugs that conflict with an individual’s allergies or other prescriptions
- Failing to give clear guidance on how to administer the medicine prescribed
- Excluding sufficient details on a prescription
Pharmacists are trained to identify if anything on a prescription looks unusual or out of the ordinary. Despite this, pharmacists and dispensers can also make mistakes themselves from time to time, such as:
- Mixing up patient prescriptions
- Incorrectly labelling medication
- Storing drugs at the incorrect temperature, or neglecting to inform patients how to store their medication at home
- Supplying fake medication, or not regulating suppliers who may provide fake/incorrect medication
- Failing to challenge a prescription they believe is inappropriate or potentially harmful
If you or someone you love suffered physically, emotionally or financially as a result of these errors, speak to our solicitors about making a wrong prescription claim.
What are the consequences of a prescription error?
In more than 75% of prescribing errors, no harm comes to the patient in question. However, it is possible for people to suffer long-term damage from prescription mistakes.
If an individual receives an excessive dosage, this could increase the likelihood that they experience side effects, or intensify the impact these adverse reactions have. On the other hand, if the dosages are too small or infrequent, or the incorrect drug is prescribed, it could mean that an individual’s underlying condition is not treated, causing them further, avoidable harm.
In extreme cases, receiving the wrong medicine can unfortunately lead to fatalities due to a severe allergic reaction. While this outcome is very rare, it is important to be aware of the impact prescription drug errors can have.
How do you prove negligence in a medication error claim?
If you suspect you or your loved one’s suffering was due to a prescription error, three key questions must be answered to prove you have a valid medical negligence claim:
- Did your healthcare provider breach their duty of care towards you?
- Did you suffer pain, injury, financial loss or damage?
- Was your suffering directly caused by your healthcare provider’s breach of duty?
As part of this process, our specialist medical negligence solicitors will gather and assess all available evidence connected to your claim, including medical records, personal statements, photographs and more.
We will also consult impartial medical experts to determine whether the actions of those responsible fell short of expectations, and quantify the impact of this negligence.
If you would like to learn more about how we can prove and support your claim for medication errors, visit our dedicated claims process page.
How much compensation can I claim for a prescription error?
As the impact of medication errors can vary significantly, so can the value of your claim. In the most serious cases, prescription-related mistakes can result in settlements of over £1 million.
Ultimately, the final settlement you receive will vary depending on the specifics of your case – such as the extent of the negligence caused and its long-term ramifications.
Compensation aims to help you get back to where you were before the negligence occurred, or if this is not possible, support changes to your life moving forward. As a result, if your claim is successful, the resulting compensation can be used to cover a wide range of costs including:
- Further medicine or treatments
- Loss of earnings while recovering from the effects of a prescription error
- Future financial losses
- Any necessary equipment or aids
- Therapies or support for any psychological harm caused
- Paying for services you or your loved can no longer perform (e.g. gardening or household chores)
- Any adaptations required to your home or vehicles
What is the time limit for filing a prescription error claim?
Like all medical negligence cases, there is a time limit of three years from the date the mistake is realised to make a claim. There are exceptions to this rule – claimants under the age of 18 have until their 21st birthday to make a claim, while there is no time limit for those who are mentally incapacitated.
The time limit does not necessarily start from the date the medication was issued or prescribed. It may be several weeks or months until you or someone you know recognises that something is wrong. This is called the date of knowledge and it ensures a claimant’s countdown begins only when they should have reasonably suspected negligence occurred, instead of when the mistake happened.
It is also helpful to know that every medical negligence claim is at the discretion of the Court, meaning it is possible for a claim to proceed even if the time limit has expired. Get in touch to set up a free initial consultation with our specialist solicitors for prescription negligence, and we will advise on whether you have a viable claim.
Contact our expert prescription and medication error claims solicitors
If you or someone you care about has been affected by a medication error, speak to our team about your options. We are here to listen and advise you on your next steps.

Lexcel accredited medical negligence claims solicitors
We are proud to be a Lexcel-accredited practice. The accreditation is a mark of quality and comes directly from the Law Society.
A recent assessment described us as a “Centre of Excellence” and we continue to operate to the highest standards across all main areas of our field. These include client care, case management, financial management, structure and strategy, people management, risk management, information management and file management.