- Home >
- MRSA Claims
When we go to the hospital, we expect to leave feeling better than when we arrived. We don’t expect to develop an infection that puts our health at greater risk. If poor hospital care caused you or a loved one to contract MRSA or led to substandard treatment of your infection, you may be eligible to file a claim.
With over 30 years of experience in all forms of medical negligence claims, our specialist solicitors fight for your right to justice. We’ve recovered millions for our clients who have suffered from negligent medical care, and can help you secure the compensation and answers you need to move on from this difficult experience.
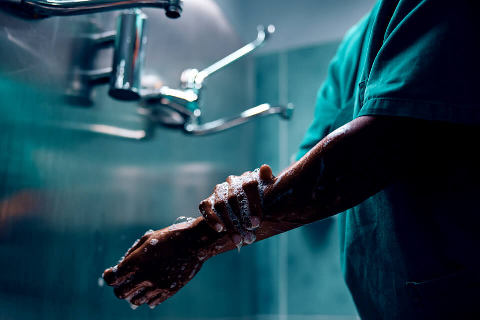
Do you have an MRSA negligence claim?
MRSA is a “superbug” that is highly resistant to antibiotics and can be fatal. It usually affects people with weakened immune systems, with hospital patients a major risk group.
If hospital staff failed to follow hygiene standards causing you or a loved one to contract MRSA, or your treatment was mishandled or delayed, our medical negligence solicitors will support your claim from start to finish.

The specialist MRSA claims solicitors for Essex & East Anglia
Whether you developed MRSA as a result of poor hospital hygiene or your infection was misdiagnosed or treated incorrectly – we are the team you can trust to get the justice you deserve.
Since 1993, Gadsby Wicks has empowered our clients to regain control over their lives and achieve true financial security. Working on a strict ‘no win, no fee’ basis, we investigate all evidence and work with relevant experts to prove your claim, with 96% of our claims settled outside of court.
What does our MRSA claim process look like?

A free initial consultation
Call us, request a callback or complete our online form and we’ll assess if you have a valid medical negligence claim.

Funding your claim
Discover the ways we can fund your claim without you paying a penny at any stage of the process.

Investigating evidence
We gather medical records, witness statements and more to learn what happened to you and prove your claim.

Instructing independent medical experts
We work with impartial, experienced medical experts to establish whether your injuries were due to substandard medical care.

Valuing your claim
We assess your health and financial losses to accurately estimate how much compensation your claim is worth.

Presenting your case
We contact the Defendants and the Courts on your behalf to set out your allegations and receive a response.

Negotiating a settlement
We work to achieve a fair settlement for you outside the courtroom – this is how 96% of our cases end.

Preparing for Trial
If we must proceed to Trial, we fully prepare you for what to expect so you receive the right result in court.
FAQs about MRSA negligence claims
What is MRSA?
MRSA (Methicillin-Resistant Staphylococcus Aureus) is a type of bacteria that can cause several harmful, hard-to-treat infections in patients. Unlike other staph infections, MRSA is trickier to treat because it has developed resistance to many antibiotics. This makes it one of the world’s most infamous ‘superbugs’ alongside Clostridium Difficile, MSSA and Klebsiella.
There are two main types of MRSA infection:
- Skin/soft tissue infections, often resulting in boils, abscesses and cellulitis
- Invasive infections deeper inside the body that may prove fatal
The MRSA bacteria live on around 1 in 30 people in the UK, usually growing in areas such as the nose, armpits, groin or buttocks in a process known as ‘colonisation’. While it lives on the surface of the skin, it is typically harmless to these individuals.
MRSA can cause numerous complications for patients who contract it, including:
- Blood poisoning
- Pneumonia
- Endocarditis
- Urinary tract infections

What are the symptoms of MRSA?
Common symptoms of MRSA include:
- Inflammation and swelling of an infected wound
- A wound feeling warmer or more painful than usual
- Development of pus
- High temperature
- Chills
- Increased heart rate and rapid breathing
- Clammy skin
- Aches and pains throughout the body
- Dizziness
- Confusion
How is MRSA treated?
Doctors treat MRSA with antibiotics. However, like other superbugs, MRSA resists many forms of antibiotics, meaning doctors must administer specific medication to treat this condition. Depending on the severity of the infection, the treatment can last from a few days to a few weeks, and healthcare providers may isolate the affected person to prevent the spread of the infection.
Infected wounds may require the patient to undergo debridement and even a skin graft. The infection may also develop into sepsis or septicaemia (blood poisoning), which is extremely dangerous and potentially fatal.
How could I contract MRSA in a hospital or similar healthcare setting?
MRSA is a serious risk in hospitals, nursing homes and other healthcare settings, as many patients are more susceptible to this type of infection:
- Patients with some form of open wound or entry point for the bacteria to enter their bloodstream
- Patients with weakened immune systems, such as if they are unwell, are elderly, are a baby or have a condition such as diabetes
- Patients surrounded by other patients and doctors who may spread disease by touching someone with the bacteria and passing it onto someone else’s skin
Examples of how MRSA may be contracted in a hospital include:
- Failure to properly cover a patient’s open wounds
- Failure to remove MRSA bacteria on a person’s skin during their hospital stay
- Failure to screen other patients for MRSA
- Failure to disinfect surfaces and objects that may have been in contact with MRSA
- Failure to wash hands between visits to different patients
- Failure to follow designated hygiene procedures
Hospitals follow strict NICE hygiene protocols designed to minimise the risk of patients contracting MRSA. Unfortunately, people do not always follow these guidelines.
If you believe you or someone you loved contracted MRSA due to the negligence of your medical professionals, start your claim today with Gadsby Wicks.

How can I prove my MRSA infection is due to medical negligence?
To prove that your MRSA infection was caused by medical negligence, you must answer three crucial questions:
- Did a medical professional breach their duty of care to me?
- Did I suffer pain, injury, financial loss or damage?
- Was my suffering directly caused by my medical professional’s breach of duty?
For a claim to be successful, it must satisfy all three of these criteria on the Balance of Probabilities (i.e. it is more likely to be true than not).
As specialist medical negligence solicitors, we help our clients prove negligence in MRSA cases, ensuring they secure the compensation, answers, and justice they deserve.
View our National and Essex Medical Negligence Statistics post for more industry insight.
Who can make an MRSA negligence claim?
Claims for MRSA negligence will typically fall into one of the following two categories:
- Negligent acquisition of MRSA
- Negligent treatment of MRSA
As noted in “How could I contract MRSA in a hospital or similar healthcare setting?”, it is possible to claim if you believe that your healthcare providers failed to put suitable hygiene measures in place, causing you to contract MRSA.
However, to make this type of claim, you must prove:
- The claimant contracted MRSA while in the hospital
- There was a failure in hygiene or other procedures
- The claimant wouldn’t have contracted MRSA without the identified failure in hygiene or other procedure
Determining a point of contraction and the actions (or inactions) that led to it is often difficult even after thorough investigation, but we have helped clients recover compensation in these circumstances.
The most common form of MRSA negligence claim involves inappropriate or substandard treatment for the infection, leading to injury or financial loss. These situations may include:
- Misdiagnosis or a delayed diagnosis of MRSA
- Delayed treatment of MRSA once identified
- Being operated on when there was awareness you had the infection
- Not receiving the correct antibiotics to treat MRSA
- Not following relevant precautions relating to your infection
Whether you or someone you care for believes they contracted MRSA from substandard hygiene procedures, or treatment of your infection was inappropriate, our specialist solicitors are ready to take on your mismanaged infection claim. Reach out to our firm today to start your journey.
Contact our expert MRSA negligence claims solicitors
If you or a loved one contracted MRSA due to negligent care, or received poor treatment for a hospital-acquired infection, speak to our team. We are here to listen and advise you on your next steps.

Lexcel accredited medical negligence claims solicitors
We are proud to be a Lexcel-accredited practice. The accreditation is a mark of quality and comes directly from the Law Society.
A recent assessment described us as a “Centre of Excellence” and we continue to operate to the highest standards across all main areas of our field. These include client care, case management, financial management, structure and strategy, people management, risk management, information management and file management.